Blog
Diabetes Drives Workers' Comp Costs, but You Can Mitigate Them
November is National Diabetes Awareness Month, which offers an opportunity to examine not only how our personal lifestyles impact diabetes risk, but also how this disease affects organizational bottom line, and what businesses can do to lessen its effect. While diabetes has broad-reaching impacts, the focus of this article is on diabetes as an unexpected workers' compensation (WC) cost, and how implementing workplace health and wellness initiatives can help offset it.
| Diabetes Costs the Healthcare System $327 Billion Annually |
We all know the high cost of diabetes to the healthcare system. Statistics from the CDC indicate a $327 billion annual cost, including a $237 billion direct medical cost of diabetes. An additional $90 billion is estimated as an indirect cost—that of lost productivity. But did you know that diabetes also costs extra in WC by complicating and worsening WC injuries? Read on for some examples of how diabetes can seep into WC claims.
Diabetes-Related Workers' Comp Claims
A common scenario involves injuries to the foot or ankle, such as a sprain, fracture, laceration, or crush injury, with preexisting diabetes. Poor blood circulation and nerve damage caused by diabetes can greatly compound even small foot injuries, threatening a host of problems, including amputation from a severe infection at worst and slowed healing at best. For the same reason, burn injuries are particularly problematic.
Preexisting diabetes in eye injuries can lead to accelerated diabetic-related eye diseases, including blindness.
| Injuries to the appendages and eyes can be exacerbated by diabetes. |
Work injuries to the feet and upper extremities can aggravate preexisting pain already caused by diabetes, such as tingling, neuropathy, and numbness. It can also make it difficult for doctors to separate the causes of overlapping symptoms, what is due to the diabetes versus the work injury.
Injuries to any body part requiring surgery run the risk of diabetes-related surgical complications and delayed recovery. A doctor can choose to postpone a surgery until a patient brings their diabetes under control. While the claims administrator is not required to pay for the diabetes treatment, they are required to pay ongoing temporary disability while waiting for the employee to act.
The Pain Points of Diabetes in Workers' Comp Claims
NCCI sample data collected for injuries with a comorbidity (two or more diseases) between 1996-2007 shows the pain points of diabetes in WC claims. These claims have almost three times the number of medical visits and eight times the number of transactions compared to claims without such diagnosis. Claim costs are also at least 25% higher.
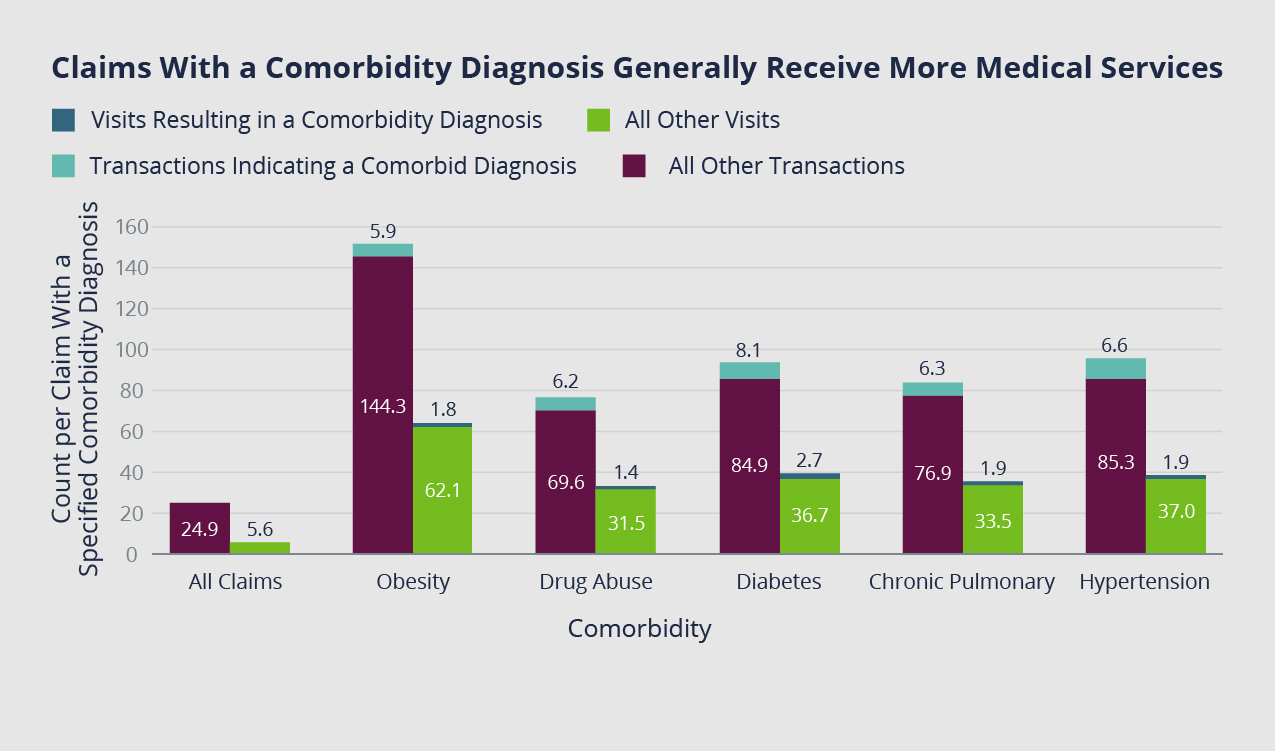
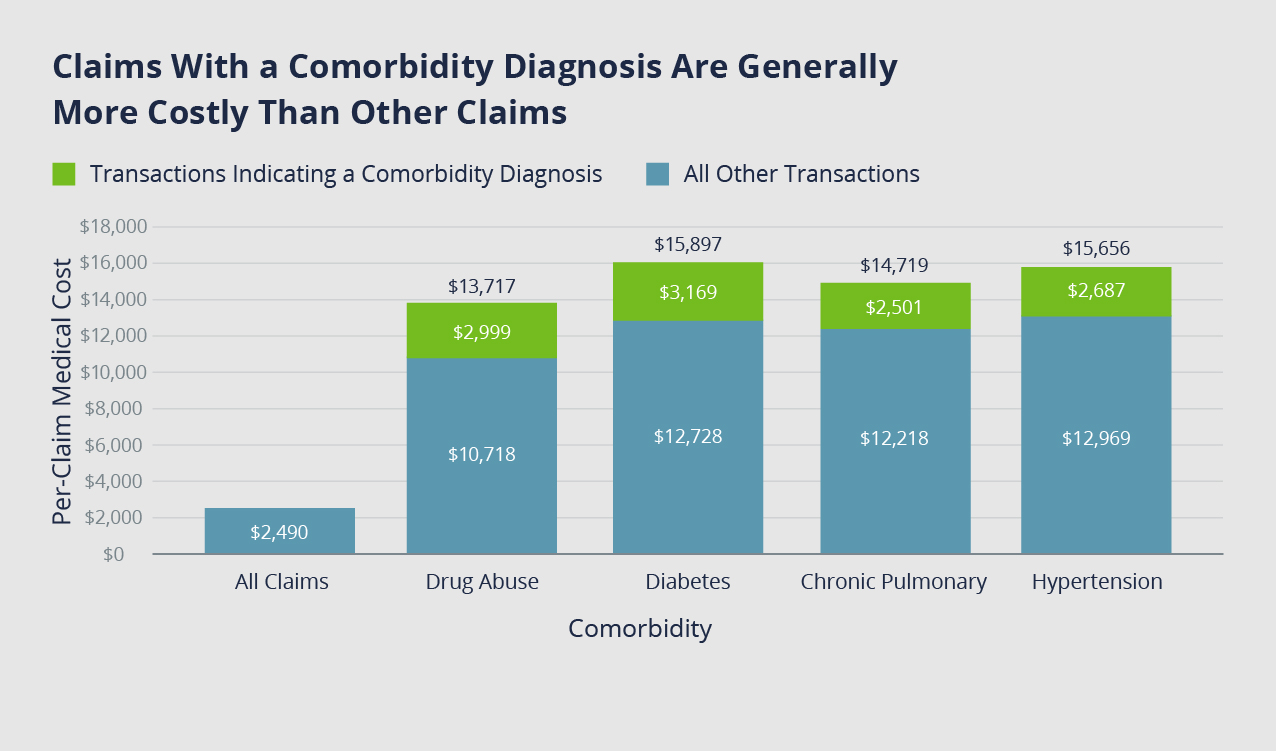
Apportionment: Separating Diabetes from the WC Injury
| Apportionment is the process used to separate an injured worker's work-permanent disability gotten at work from a disability received outside of work. |
Apportionment is used by claims administrators to tease out non-industrial factors that add to claim costs. There are challenges to this approach, however. First, legally, apportionment can only be applied to permanent disability (PD), which is not addressed until the final stages of a claim, after lengthy and costly temporary disability (TD) and medical treatment, the bulk of most claim costs, have already been spent. The monetary difference, after factoring for apportionment, is often minimal.
Apportionment is not just driven by WC physicians. It is also a legal issue with a complex set of rules and requires workers’ compensation board approval. This makes it difficult for doctors to get away with assigning large percentages of apportionment. Oftentimes the litigation expenses incurred to continue fighting for apportionment eat up any potential cost savings.
As in all other claim legalities, apportionment is subject to different regulations across the 50 states. Some states limit apportionment to certain types of factors. Earlier this year, California almost adopted a regulation prohibiting apportionment based on aging factors. Though Governor Newsom vetoed it, this is probably not the last time the issue will be raised.
Some states require evidence that the preexisting condition was disabling prior to the injury. Some even require that the condition was specifically from a prior WC injury that had a disability settlement. Variations imposed in other states offer little to no apportionment protection based on a whole person premise, meaning WC must treat the entire person, not solely the injured body part(s).
Focus on Prevention
While claims administrators should continue efforts to build strong apportionment defenses when appropriate, there need to be other solutions to underlying diabetes in WC claims. Why not turn the tide from a reactionary approach to one that is proactive? An ounce of prevention is worth a pound of cure. Employers who concentrate their awareness, efforts, and resources on workplace health and wellness are using one such preventative strategy.
In fact, the focus of this year’s diabetes awareness month is on prevention and prediabetes. It is estimated that 34% of adults have prediabetes, which is a lifestyle preventable and reversible condition.
Offer Resources to Reduce the Risk of Diabetes
If employers understand the factors associated with an increased risk of prediabetes and diabetes (particularly type 2), such as lack of physical activity and smoking, they can begin to educate their workforce and take preventative measures—such as encouraging exercise, smoking cessation (where indicated), and proper nutrition—in order to reduce the risks.
First, if you have a wellness calendar (start one if you don’t), make sure to highlight November as National Diabetes Awareness Month. Consider sending employees this link from the CDC—a great resource for starting a diabetes education program.
Further, if you’re helping employees snack on nutrient-rich foods by providing fresh fruits and vegetables rather than sugar-loaded vending machines, you’ve already started a positive trend. Putting up a diabetes prevention poster in your lunch breakroom is another awareness-raising environmental tactic.
A great way to encourage both fitness and team building is to start an in-person or virtual walking program. Some companies form teams through apps like Charity Miles, an organization that partners with corporate sponsors to raise money for charities through movement. You could also offer biometric screening and HRAs (health risk assessments) that may help employees identify their baseline as well as modifiable lifestyle risk factors. Even with a limited budget, there are numerous little-to-no-cost strategies, such as starting a healthy eating or exercise Slack channel or Employee Resource Group (ERG), or one that combines multiple topics as part of diabetes prevention.
Partner with Services and Platforms to Promote Health
Partnering with a service like Freshly to pay for or subsidize healthy meal subscriptions is something that could be done for remote workers. There are also apps to tell your employees about, even free ones, that provide information, recipes, and exercise videos. One such app, Mindmate, though designed with brain health in mind, features recipes based on the evidence-based MIND diet adapted from the Mediterranean diet. This diet, combined with a healthy lifestyle, not only improves brain function, but crosses over to diabetes prevention. Incidentally, Alzheimer’s disease is being dubbed “diabetes type 3.”
Investing in a digital platform, such as Wondr Health, a behavioral change program, has enabled employers to help employees reduce health conditions such as diabetes and improve overall physical and mental wellness.
Changing health and wellness culture in the workplace is not an overnight task. It may take years of building awareness and participation and implementing and monitoring strategies before you see results. However, with consistent measures over the long term, you can expect to see lower WC and healthcare costs as well as more productive and happier employees. By helping your employees focus on healthy lifestyle behaviors to reduce diabetes risk, you are helping them lower the risk of other biopsychosocial factors, such as heart disease and depression, which also impact WC claims.
Read our latest property and casualty looking ahead guide where we forecast upcoming trends, including workers' compensation considerations, the impact of the pandemic, accelerating climate changes, and litigation trends.
Author
Table of Contents














